Gallbladder Cholecystitis
Perforated Cholecystitis Neglected cholecystitis evolves into gallbladder perforation. Most perforations are walled-off and result in pericholecystic fluid or a right upper quadrant abscess, a common location being between the gallbladder and adjacent liver. Free perforation into the peritoneal cavity results in bile peritonitis, while an occasional perforation into the liver evolves into a liver abscess. Chronic perforations have evolved into a cholecystocutaneous or cholecystoenteric fistula, and even a cholecystogastric fistula. Detection of gallbladder perforation is not straightforward. Adherent omentum, fat, or adhesions often mask a recent perforation. Computed tomography visualizes only about half of gallbladder wall defects, and US even less. Pericholecystic fluid and gallbladder wall thickening are often the only pertinent imaging findings.
Radiology images of Spontaneous cholecystocutaneous fistula (arrow) secondary to cystic duct obstruction by a stone.
Gangrenous Cholecystitis
Gangrenous cholecystitis is a sequela of either calculus or acalculus cholecystitis. Computed tomography and US reveal similar findings. The gallbladder wall is irregular and thick. Sloughed gallbladder mucosa is seen as thin intraluminal linear echoes parallel to the gallbladder wall and a striated wall edema pattern seen with US should suggest gangrenous cholecystitis. Often inflammation extends to surrounding structures. A sonographic Murphy’s sign is less often elicited in
these patients than with more conventional acute cholecystitis. Color Doppler US reveals no flow within a thickened gallbladder wall in acute necrotizing cholecystitis. Occasionally a thin rim of increased scintigraphic activity, a rim sign, is seen adjacent to the gallbladder fossa, a sign associated with gallbladder wall gangrene. The presence of arim sign, together with subsequent gallbladder visualization after administration of morphine, does occur with gallbladder gangrene. The rim sign should be distinguished from tracer activity in adjacent liver parenchyma.
Empyema/Abscess
Empyema, consisting of an obstructed, pusfilled gallbladder lumen, leads to marked gallbladder distention. Ultrasonography shows a markedly distended, hyperechoic sludgecontaining gallbladder. Computed tomography reveals this pus-filled gallbladder content to have greater attenuation than bile. At times a frank abscess is identified. Laparoscopic cholecystectomy is difficult in the setting of gallbladder empyema and many of these patients undergo conventional cholecystectomy.
Empyema, consisting of an obstructed, pusfilled gallbladder lumen, leads to marked gallbladder distention. Ultrasonography shows a markedly distended, hyperechoic sludgecontaining gallbladder. Computed tomography reveals this pus-filled gallbladder content to have greater attenuation than bile. At times a frank abscess is identified. Laparoscopic cholecystectomy is difficult in the setting of gallbladder empyema and many of these patients undergo conventional cholecystectomy.
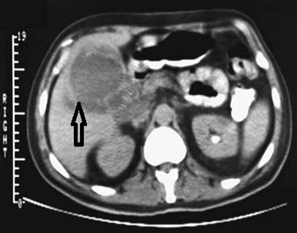
Radiology images of Salmonella cholecystitis resulting in a gallbladder abscess (arrow).The abscess was drained percutaneously.
Emphysematous Cholecystitis
Emphysematous cholecystitis is a severe form of acute cholecystitis manifesting with gas (not air) in the gallbladder lumen, wall, bile ducts, or pericholecystic tissues, and no abnormal communication between the biliary tree and gastrointestinal tract. It develops if gas-forming bacteria predominate as the infectious organism. Diabetes mellitus is a common underlying condition. Some of these patients do not appear systemically ill, and unless imaging suggests the condition, conservative therapy may be initially initiated. Nevertheless, mortality is about 15%. Gallstones are absent in some of these patients. In some, a superimposed pneumoperitoneum suggests a perforation. Rarely, simultaneous emphysematous pyelonephritis and emphysematous cholecystitis develop.
The diagnosis is straightforward with conventional radiography and CT, revealing gas in the gallbladder lumen, wall, or pericholecystic tissues. Ultrasono-graphy can miss emphysematous cholecystitis due to gallbladder nonvisualization; intramural gas can be confused with gas within the bowel. If the gallbladder is identified, US reveals highly reflective echoes from nondependent gallbladder wall segments. Exten-sive gas mimics gallbladder wall calcifications. Ultrasonography in one patient revealed gas bubbles rising within the gallbladder and floating to the surface, an appearance called effervescent gallbladder. Cholescintigraphy may or may not detect cystic duct obstruction in these patients. Although successful percutaneous gallbladder drainage has been performed in these patient, most are managed surgically.
Emphysematous cholecystitis is a severe form of acute cholecystitis manifesting with gas (not air) in the gallbladder lumen, wall, bile ducts, or pericholecystic tissues, and no abnormal communication between the biliary tree and gastrointestinal tract. It develops if gas-forming bacteria predominate as the infectious organism. Diabetes mellitus is a common underlying condition. Some of these patients do not appear systemically ill, and unless imaging suggests the condition, conservative therapy may be initially initiated. Nevertheless, mortality is about 15%. Gallstones are absent in some of these patients. In some, a superimposed pneumoperitoneum suggests a perforation. Rarely, simultaneous emphysematous pyelonephritis and emphysematous cholecystitis develop.
The diagnosis is straightforward with conventional radiography and CT, revealing gas in the gallbladder lumen, wall, or pericholecystic tissues. Ultrasono-graphy can miss emphysematous cholecystitis due to gallbladder nonvisualization; intramural gas can be confused with gas within the bowel. If the gallbladder is identified, US reveals highly reflective echoes from nondependent gallbladder wall segments. Exten-sive gas mimics gallbladder wall calcifications. Ultrasonography in one patient revealed gas bubbles rising within the gallbladder and floating to the surface, an appearance called effervescent gallbladder. Cholescintigraphy may or may not detect cystic duct obstruction in these patients. Although successful percutaneous gallbladder drainage has been performed in these patient, most are managed surgically.
Radiology images of Emphysematous cholecystitis. Radiograph (A) and CT (B) in two different patients.Gas is present in the gallbladder wall and lumen (arrow). Pneumobilia was identified on other images.
Eosinophilic Cholecystitis
Histologically, eosinophilic cholecystitis consists of a transmural eosinophilic infiltrate. It is associated with allergic conditions, parasites, hypereosinophilic syndromes, and even with calculous acute cholecystitis. Tissue infiltration with eosinophils and eosinophilic granulomas occurs in necrotizing granulomatous vasculitis involving the gallbladder; similar features are found in allergic granulomatous angiitis of Churg and Strauss.
Histologically, eosinophilic cholecystitis consists of a transmural eosinophilic infiltrate. It is associated with allergic conditions, parasites, hypereosinophilic syndromes, and even with calculous acute cholecystitis. Tissue infiltration with eosinophils and eosinophilic granulomas occurs in necrotizing granulomatous vasculitis involving the gallbladder; similar features are found in allergic granulomatous angiitis of Churg and Strauss.
Therapy
In Pregnancy, Traditionally, a pregnant woman with acute cholecystitis has undergone an open cholecystectomy, although a laparoscopic cholecystectomy
is feasible. If warranted, cholangiography is performed. A pneumoperitoneum is induced during a typical laparoscopic cholecystectomy; gasless laparoscopic cholecystectomy has been performed in pregnant women.Ultrasonography-guided percutaneous cholecystostomy may have a role in pregnancy; biliary decompression is maintained during pregnancy and an elective cholecystectomy performed after delivery.


Post a Comment for "Gallbladder Cholecystitis"